
Early diagnosis would allow to plan personalized and appropriate therapeutic and rehabilitative pathways, minimizing the negative impact due to TMD. The present study suggests that all patients with TMD should be investigated for new-onset otological symptoms, regardless of oral parafunctional habits. No significant correlations were found between tinnitus and bruxism (p = 0.28), clenching (p = 0.11), nail-biting (p = 0.96), sleeping prone (p = 0.27), chewing gum (p = 0.99) and talking for a long time (p = 0.42). Among otological symptoms, aural fullness was the most common (n = 133, 33.3%), followed by tinnitus (n = 92, 23%) and vertigo (n = 79, 19.8%). Overall, new-onset otological symptoms were reported by 304 (76%) subjects with TMD. A total of 400 patients (301 females, 99 males) met the inclusion criteria, with a median age of 39.6 ± 15.6 years. Tinnitus was also analyzed in more detail to evaluate possible associations with parafunctional habits. The medical reports and charts of patients who experienced TMD between 1 February 2016 and 31 December 2017 were reviewed, in order to evaluate the prevalence of new-onset aural fullness, vertigo and tinnitus. The aim of this retrospective study was to evaluate the prevalence of new-onset otological symptoms and the possible associations between tinnitus and oral parafunctional habits among patients with temporomandibular disorders (TMD) who attended a Craniofacial Pain Outpatient and a Dentistry Clinic. Patients gave informed consent preoperatively, and reassurance postoperatively is prudent. The risk of minor changes in hearing function is probable during the first week after orthognathic surgery, but these negative changes will either totally fade or remain negligible. Negative changes were found in the results of ETFT in vertical movements, which returned to pre-surgery values in the final test. No significant difference was also observed between horizontal and vertical movements in the results of tympanometry. In other words, no significant changes occurred in patients’ hearing threshold after surgery. PTA evaluation, based on horizontal or vertical movements, did not show significant differences, although vertical movements resulted in less change in hearing threshold. Patients were tabulated based on the type of maxilla and mandibular surgical movements (vertical and horizontal). 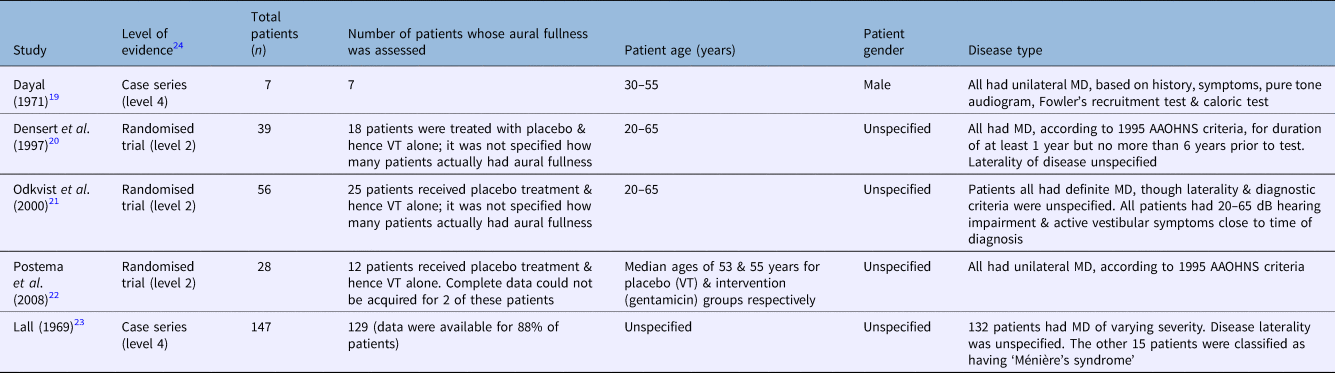
Pure tone audiometry (PTA), tympanometry, and Eustachian Tube Dysfunction Test (ETFT) were performed postoperatively at 24 h, 6 weeks, and 6 months after surgery. Patients underwent either single or double jaw surgery. Thirty-one orthognathic surgery candidates were recruited in this study. This study aimed to evaluate the potential changes in orthognathic surgery on the hearing function of patients. 
Any surgical procedure could cause side effects. Orthognathic surgery is widely used in treating functional and skeletal problems. TMD as a potential cause of aural fullness should be considered in otolaryngology practice. TMD treatments are especially effective (94.1%) in group I TMD. Aural fullness was completely resolved or significantly improved in 67 and 34 patients respectively following treatments aimed at improving TMD, with a combined effectiveness of 90.2% (101/112). The patients of 60.7% (68/112) were classified as group I TMD disorders (muscle disorders), 34.8% (39/112) were group II (disc displacements), and 4.5% (5/112) were group III (arthralgia, osteoarthritis, and osteoarthrosis). Patients were then treated for TMD.Īll the patients showed normal eardrum and type A tympanogram. TMD was categorized according to the Research Diagnostic Criteria for Temporomandibular Disorders (RDC/TMD). Patients were examined by questionnaire, X-ray and/or computed tomography scan of temporomandibular joint. Patients were subjected to pure tone audiometry and acoustic immittance screening using GSI-61 clinical audiometer and GSI TympStar middle ear analyzer respectively. Patients' medical history indicated that they had previously been diagnosed and treated for otitis media or sensorineural hearing loss but without positive results. One hundred and twelve patients, who had aural fullness as the main or sole complaint, presented to the Otolaryngology Department, PLA Army General Hospital, Beijing, China, between January 2010 and January 2015. 
The purpose was to investigate the TMD and effectiveness of TMD treatments in patients with mainly or exclusively aural fullness complaint. However, it is not clear whether aural fullness could be induced by TMD. Temporomandibular joint disorders (TMD) are often associated with aural manifestations.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
